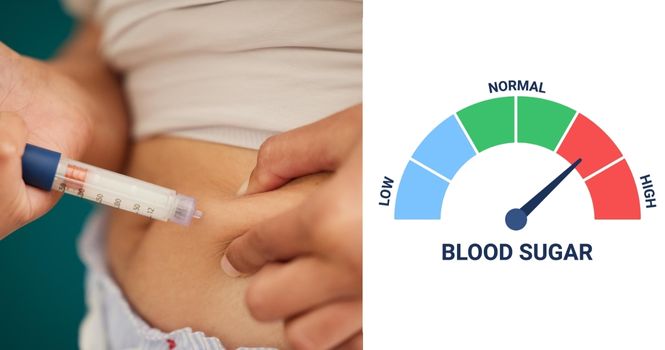
Do you have Sugar? Is a phrase people frequently ask elders, while offering sweets on any occasion.
This term, “Sugar” has become synonymous with Diabetes. Lets Understand Sugar and Blood Sugar Levels, not only in older adults but in every age group.
Why is Sugar so important to the Human Body?
Sugar, specifically Glucose, plays a vital role in the functioning of the human body. The important reasons are;
1. Primary Energy Source:
Glucose is the body’s primary source of energy. It’s used by every cell to power its functions. The brain, in particular, relies heavily on glucose to carry out its tasks.
2. Glycogen Storage:
When you have an abundance of glucose, your body can convert it into a substance called glycogen. This is stored in your liver and muscles, and can be quickly converted back to glucose when needed for energy, as in between meals or during a sudden brief sprint.
3. Fuel During Exercise:
During high-intensity exercise, your body burns glucose to keep your muscles working. Glycogen stores are particularly important for endurance athletes, as these stores can be drawn upon when glucose levels drop.
4. Metabolic Processes:
Glucose plays a role in various metabolic processes. For example, it is involved in the synthesis of certain amino acids and the creation of other sugars needed by the body.
It’s important to understand that while sugar is essential for the body’s functioning, too much sugar, particularly in the form of added sugars in processed foods and drinks, can lead to health problems such as obesity, type 2 diabetes, and heart disease.
Balance and moderation are key. The body needs sugar, but it’s important to provide it in a healthy way, primarily through a diet rich in whole foods like fruits, vegetables, and whole grains.
How Much Milligrams of Sugar is Present in Blood of Normal Healthy Individuals?
The average human adult contains around 5 liters of Blood, depending on many factors.
In the United States, blood glucose concentration is typically measured in milligrams per deciliter (mg/dL), while many other countries use millimoles per liter (mmol/L).
Normal fasting blood glucose levels in a healthy individual typically range between 70 to 100 mg/dL, or approximately 3.9 to 5.5 mmol/L.
Let’s calculate the total amount of glucose in 5 liters of blood using the upper limits for both measurements:
Using mg/dL:
100 mg/dL * 50 dL (since there are 10 deciliters in a liter, and we have 5 liters) = 5000 mg or 5 grams of glucose.
Using mmol/L:
5.5 mmol/L * 5 L = 27.5 mmol of glucose.
So, in 5 liters of blood, a healthy individual would typically have around 5000 milligrams (or 5 grams) of glucose, which is approximately 27.5 millimoles.
This is an estimation, as actual blood glucose levels can vary based on many factors including diet, physical activity, and overall health status.
So it’s only 5 grams in your Blood.
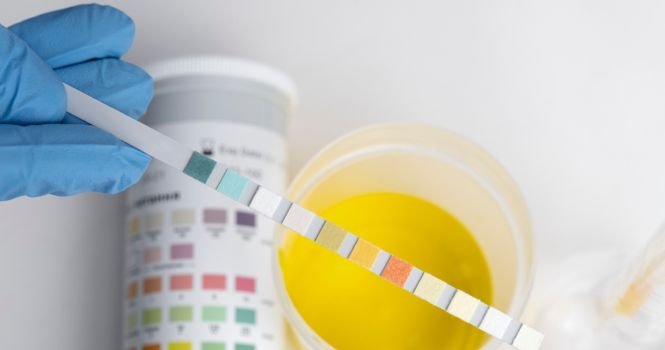
How is Blood Sugar Measured?
Blood sugar, also known as blood glucose, is measured in several ways, usually via a blood test. The Blood is taken from a Vein and following tests are commonly done.
1. Fasting Blood Sugar Test:
This test measures your blood sugar after an overnight fast (not eating for at least 8 hours). It’s often the first test done to check for prediabetes and diabetes.
2. Post Prandial Sugar Test:
This test is performed after 90 to 120 minutes after breakfast and is also called Post Lunch Blood Sugar test.
3. Random Blood Sugar Test:
This test is exactly as it sounds. A blood sample is taken at a random time, regardless of when you last ate. A random blood sugar level of 200 milligrams per deciliter (mg/dL) or higher suggests diabetes.
4. Oral Glucose Tolerance Test (OGTT):
For this test, you will fast overnight, and the fasting blood sugar level is measured. Then you drink a sugary liquid as advised by your doctor (50g Glucose or 75g Glucose mixed with water) and blood sugar levels are tested periodically for the next two hours, every hour.
5. A1C Test (Glycated Hemoglobin Test):
This test indicates your average blood sugar level for the past three months. It measures the percentage of your hemoglobin (a protein in red blood cells) that is coated with sugar.
The higher your blood sugar levels, the more hemoglobin you’ll have with sugar attached. An A1C level of 6.5 percent or higher on two separate tests indicates diabetes.
Units of Measurements of Blood Sugar
The standard blood sugar levels are measured in milligrams per deciliter (mg/dL) or millimoles per liter (mmol/L). This measurement can vary depending on the country and the specific laboratory.
We have personal or home glucose monitors available for people with diabetes. These devices allow people to track their blood sugar levels throughout the day.
They work by pricking your finger for a small blood sample, which is then applied to a test strip inserted into the device.
Difference Between Glucose Challenge Test and Oral Glucose Tolerance Test
| Glucose Challenge Test (GCT) | Oral Glucose Tolerance Test (OGTT) | |
| Purpose | Screens for gestational diabetes; usually performed between 24 and 28 weeks of pregnancy | Diagnoses gestational diabetes, prediabetes, and type 2 diabetes |
| Preparation | No fasting required | Requires an 8-12 hour fast prior to the test |
| Procedure | A sweet drink containing 50 grams of glucose is consumed, followed by a blood test after 1 hour | After fasting, blood is drawn, a drink containing 50 grams of glucose is consumed, and blood is then drawn every 60 minutes for up to 3 hours |
| Interpretation | If blood glucose is above a certain threshold (usually 130-140 mg/dL), it indicates a need for the OGTT | Blood glucose levels are measured at each interval. Specific thresholds at each interval are used to diagnose prediabetes and diabetes |
What Causes Diabetes?
Diabetes is a chronic health condition where the body is either unable to produce enough insulin or cannot effectively use the insulin it produces.
Insulin is a hormone that regulates blood sugar. This leads to elevated levels of glucose in the blood, known as hyperglycemia.
Persistent hyperglycemia can damage the body’s systems, particularly the blood vessels and nerves.
Different Types of Diabetes
The most common types of diabetes are Type 1, Type 2, Gestational Diabetes, Prediabetes.
1. Type 1 Diabetes:
This form of diabetes is an autoimmune condition. It occurs when your immune system mistakenly attacks and destroys the insulin-producing cells in your pancreas.
The exact cause is unknown, but it’s thought to be a combination of genetic susceptibility and environmental factors, like viruses, that might trigger the disease.
Type 1 is divided into;
- Immune mediated Type 1 Diabetes Mellitus (Type 1A )
- Idiopathic Type 1 Diabetes Mellitus (Type 1B)
2. Type 2 Diabetes:
This type of diabetes is primarily influenced by lifestyle factors and genetics. In type 2 diabetes, your body becomes resistant to insulin, and your pancreas is unable to make enough insulin to overcome this resistance.
Overweight, obesity, physical inactivity, and poor diet can significantly contribute to the development of this type of diabetes.
3. Gestational Diabetes:
This type of diabetes occurs in some women during pregnancy when the body becomes less sensitive to insulin.
Gestational diabetes, like other types of diabetes, involves a problem with insulin regulation.
4. Prediabetes:
This is a condition where your blood sugar levels are higher than normal, but not high enough to be classified as type 2 diabetes. Without lifestyle changes, people with prediabetes are very likely to progress to type 2 diabetes.
Read more on What is Considered Prediabetes
5. Other Specific Types of Diabetes
- Maturity Onset Diabetes of the young
- Diabetes Mellitus associated with mutation of mitochondrial DNA
- Wolfram Syndrome
- Autosomal Recessive syndrome
- Diabetes Mellitus secondary to other causes
- Hyperglycemia due to tissue insensitivity to insulin
- Hormonal tumors (acromegaly, Cushing syndrome, glucagonoma, pheochromocytoma)
- Due to Drugs (corticosteroids, sympathomimetic drugs, niacin)
- Liver disease (cirrhosis, hemochromatosis)
- Muscle disorders (myotonic dystrophy)
- Truncal obesity Insulin receptor disorders (acanthosis nigricans)
- Hyperglycemia due to reduced insulin secretion
- Hormonal tumors (somatostatinoma, pheochromocytoma)
- Pancreatic disorders (pancreatitis, hemosiderosis, hemochromatosis)
- Drugs (thiazide diuretics, phenytoin
- Hyperglycemia due to tissue insensitivity to insulin
All types of diabetes lead to high blood sugar levels, if left unchecked, which can lead to serious health problems like heart disease, vision loss, and kidney disease.
The cause of diabetes varies by type, but all forms can lead to excess sugar in your blood. Too much sugar in your blood can damage various body systems and organs over time.
Remember, regular check-ups and a healthy lifestyle are essential to prevent or manage diabetes.
If you have any symptoms of diabetes such as excessive thirst, frequent urination, unexplained weight loss, constant hunger, or slow healing sores, seek medical attention immediately.
Diagnosis of Diabetes
The following Tabular column illustrates on How Diabetes is Diagnosed.
You can also Read on How different types of Diabetes are Diagnosed
| Test | Procedure | Diagnosis Criteria |
| Fasting Plasma Glucose (FPG) Test | Measures blood sugar after an overnight fast (not eating for at least 8 hours). | Fasting blood sugar level of 126 mg/dL or higher on two separate tests indicates diabetes. |
| Oral Glucose Tolerance Test (OGTT) | Involves fasting overnight, then drinking a sugary liquid and having your blood sugar levels checked over the next two hours. | Blood sugar level of 200 mg/dL or higher during this test suggests diabetes. |
| Random (Non-Fasting) Blood Sugar Test | Blood sugar level test conducted at any time, regardless of when you last ate. | Blood sugar level of 200 mg/dL or higher indicates diabetes. |
| Hemoglobin A1C (HbA1c) Test | Measures the percentage of blood sugar attached to the oxygen-carrying protein in red blood cells (hemoglobin). | An A1C level of 6.5 percent or higher on two separate tests indicates diabetes. |
Normal Sugar Level Chart in Healthy Individuals Age wise (Fasting & After Food)
| Age Group | Fasting (mg/dL) | Fasting (mmol/L) | After Eating (mg/dL) | After Eating (mmol/L) |
| Children and Adolescents (<18 years) | 70-100 | 3.9-5.6 | <140 | <7.8 |
| Adults (18 years and older) | 70-100 | 3.9-5.6 | <140 | <7.8 |
| Older Adults (65 years and older) | 70-110 | 3.9-6.1 | <160 | <8.9 |
Normal Blood Sugar Levels for Diabetic Patients, Age wise
Blood sugar levels for people with diabetes can vary widely based on the individual, their treatment plan, and the type of diabetes.
However, the American Diabetes Association has general targets for most people with diabetes, which are given in the table below,
| Age Group | Fasting (mg/dL) | Fasting (mmol/L) | After Eating (mg/dL) | After Eating (mmol/L) |
| Children and Adolescents (<18 years) | 80-130 | 4.4-7.2 | <180 | <10.0 |
| Adults (18 years and older) | 80-130 | 4.4-7.2 | <180 | <10.0 |
| Older Adults (65 years and older) | Individualized | Individualized | Individualized | Individualized |
For older adults, target levels can vary greatly due to the presence of other health conditions, the risk of hypoglycemia, and the individual’s general health status. As such, it’s recommended that blood sugar targets be individualized.
These are general guidelines, and individual targets may vary. Always consult with a healthcare provider for personalized advice and information.
It’s important to keep in mind that these are targets for self-monitoring of blood sugar levels. Clinical targets for HbA1c, a measure of long-term blood sugar control, may be different.
Random Blood Sugar Chart, Age Wise
Random blood sugar levels, also known as casual plasma glucose levels, can be measured at any time without regard to when the last meal was consumed.
They are less reliable than fasting or postprandial glucose levels for diagnosing diabetes because they are influenced by recent meals, exercise, and other factors.
However, a random blood sugar level of 200 mg/dL (11.1 mmol/L) or higher, particularly if the person also has symptoms of hyperglycemia, can indicate diabetes.
The American Diabetes Association suggests a random blood sugar target for most nonpregnant adults with diabetes of less than 180 mg/dL (10.0 mmol/L).
Unfortunately, specific normal ranges for random blood sugar levels based on age aren’t typically provided due to their less reliable nature for diagnostic purposes.
It’s always best to consult your doctor for personalized advice and information.
Following is a rough guidelines which could be of help
| Age Group | Random Blood Sugar (mg/dL) | Random Blood Sugar (mmol/L) |
| Children and Adolescents (<18 years) | <180 | <10.0 |
| Adults (18 years and older) | <180 | <10.0 |
| Older Adults (65 years and older) | Individualized | Individualized |
What is Hyperglycemia and Hypoglycemia?
Hyperglycemia
Hyperglycemia refers to high levels of glucose (sugar) in the blood. It’s a common condition in people with diabetes, both type 1 and type 2.
Under normal circumstances, your body maintains blood sugar levels within a narrow range. However, in diabetes, this regulatory system is impaired, either because the pancreas doesn’t produce enough insulin (as in type 1 diabetes) or because the body’s cells are resistant to the effects of insulin (as in type 2 diabetes).
Hyperglycemia can occur when blood sugar control in the body is not well managed.
It can also be a result of eating more carbohydrates than the body can handle, not getting enough physical activity, illness, or not taking enough diabetes medication.
Hypoglycemia
Hypoglycemia refers to abnormally low levels of glucose (sugar) in the blood, usually less than 70 milligrams per deciliter (mg/dL).
It’s most commonly a condition in people with diabetes, particularly type 1 diabetes or type 2 diabetes who are managing their condition with insulin or certain other medications.
Hypoglycemia typically occurs as a result of an imbalance between your insulin dose, the amount of carbohydrates (food) you eat, and your level of physical activity.
Too much insulin or other glucose-lowering diabetes medication, not eating enough carbohydrates, or increased physical activity can cause blood glucose to fall too low, leading to hypoglycemia.
High and Low Blood Sugar Levels With Diabetes in Adults
The following are general guidelines for blood sugar levels provided by the American Diabetes Association. However, these values can be adjusted based on an individual’s health status and the advice of your healthcare provider.
| Blood Sugar Condition | Blood Sugar Level (mg/dL) | Blood Sugar Level (mmol/L) |
| Normal | 70-130 | 3.9-7.2 |
| Preprandial Hyperglycemia | >130 | >7.2 |
| Postprandial Hyperglycemia | >180 | >10.0 |
| Hypoglycemia | <70 | <3.9 |
| Diabetic Ketoacidosis | >250 | >13.9 |
| Hyperglycemic Hyperosmolar State | >600 | >33.3 |
Please Note:
- Preprandial Hyperglycemia refers to high blood sugar before a meal.
- Postprandial Hyperglycemia refers to high blood sugar after a meal.
- Hypoglycemia refers to low blood sugar.
- Diabetic Ketoacidosis is a serious diabetes complication where the body produces excess blood acids (ketones).
- Hyperglycemic Hyperosmolar State is a serious condition that can occur in people with diabetes who do not control their blood sugar levels, leading to severe dehydration and coma.
These are just general guidelines and actual blood sugar levels can vary significantly based on a variety of factors.
Symptoms of High Blood Glucose (Hyperglycemia)
The Symptoms of hyperglycemia which are mentioned below, if left untreated, can lead to serious complications, including diabetic ketoacidosis and hyperosmolar hyperglycemic state, both of which are medical emergencies.
These symptoms can vary from person to person, and they can also depend on how high blood sugar levels are,
1. Frequent Urination:
The kidneys try to get rid of the excess glucose in the blood by flushing it out of the body through urine.
2. Increased Thirst:
The body tries to replenish lost fluids from frequent urination, leading to thirst.
3. Blurred Vision:
High blood sugar can cause the lens of the eye to swell, resulting in blurred vision.
4. Fatigue:
The body’s cells aren’t getting the energy they need from glucose, which can result in feeling tired or fatigued.
5. Frequent infections or slow-healing wounds:
High blood sugar can affect the body’s ability to heal and resist infections.
6. Unintentional Weight Loss:
If your body can’t get energy from glucose, it may start breaking down muscle and later fat for energy instead, leading to weight loss.
7. Increased Hunger:
When the body can’t use glucose properly for energy, it may cause increased feelings of hunger.
8. Dry Skin and Mouth:
Dehydration caused by increased urination can lead to dry skin and dry mouth.
9. Nausea and Vomiting:
If blood sugar levels become extremely high, a person may experience nausea and vomiting.
10. Shortness of Breath:
This symptom is more likely to occur if hyperglycemia has led to a condition called Ketoacidosis.
If you’re experiencing symptoms of hyperglycemia, it’s important to consult with your Doctor.
Chronic hyperglycemia can lead to serious complications if left untreated.
How to Lower Blood Glucose Levels?
First consult your Doctor and Get it Diagnosed, if you are unsure if you have Diabetes or Not or hovering on the borderline as in Prediabetes and thinking that you could get it down with exercise and food. Consult first.
Remember if the Blood Sugar Level is consistently High, then it could lead to complications and Blindness.
Other than Medication, which are used to lower Blood Glucose , Other Methods commonly employed are,
1. Healthy Eating: Follow a balanced, nutritious diet rich in whole grains, lean proteins, and healthy fats. Limit processed foods and sugary drinks.
2. Carbohydrate Counting: Learn to count carbs and understand how they affect your blood sugar levels. This can help you manage your glucose levels more effectively.
3. Regular Exercise: Regular physical activity can help your body use insulin more efficiently, lower your blood sugar levels, and maintain a healthy weight.
4. Medication or Insulin Therapy: Depending on the type and severity of your diabetes, you may need medications or insulin to help manage your blood sugar levels.
5. Regular Monitoring: Regularly monitor your blood sugar levels to understand how different foods, activities, and situations affect your glucose levels.
6. Weight Management: If you’re overweight, losing even a small amount of weight can improve your body’s insulin sensitivity and help control blood sugar levels.
7. Limit Alcohol: Alcohol can affect your blood sugar levels, so limit your intake and never drink on an empty stomach.
8. Quit Smoking: Smoking increases the risk of diabetes complications, including high blood sugar levels.
9. Stress Management: Stress can affect blood sugar levels. Techniques such as yoga, meditation, or other stress-reducing activities can help.
Remember, everyone is different, so what works for one person might not work for another.
It’s also crucial to have regular check-ups with your healthcare provider to make sure your blood sugar levels are within the target range set for you.
Adjustments to your treatment plan can be made as necessary.
Symptoms of Low Blood Sugar Levels (Hypoglycemia)
Hypoglycemia, or low blood sugar, occurs when your blood sugar levels have fallen low enough that you need to take action to bring them back to your target range.
It’s important to treat hypoglycemia promptly to avoid these severe symptoms, like seizures and loss of consciousness by consuming fast-acting carbohydrates like fruit juice, candy, or glucose gel.
If left untreated, hypoglycemia can be life-threatening.
The common symptoms of hypoglycemia are,
1. Shakiness or nervousness: This is often one of the first signs of hypoglycemia. Your body is signaling that it needs more glucose.
2. Sweating: You may experience sudden, excessive sweating even when you are not exercising or in a warm environment.
3. Hunger: Despite eating regular meals, you might feel a strong urge to eat because your body is seeking more energy.
4. Irritability or mood swings: Low blood sugar can affect your mood and may cause you to become suddenly irritable or moody.
5. Dizziness or light-headedness: This may occur if your brain isn’t getting enough glucose to function properly.
6. Fatigue or weakness: Without enough glucose, your body may not have enough energy, which can result in feeling tired or weak.
7. Headache: Low glucose levels can cause headaches in some people.
8. Trouble concentrating or confusion: Your brain needs a steady supply of glucose to function properly, so hypoglycemia can make it difficult to focus or make you feel confused.
9. Blurred vision or seeing double: Just like hyperglycemia, hypoglycemia can also affect your vision.
10. Loss of consciousness, seizure, or coma: These are severe symptoms that occur when blood sugar levels become extremely low.
It’s important to treat hypoglycemia as soon as possible to prevent more severe symptoms from occurring.
If you frequently experience symptoms of hypoglycemia, or if you aren’t sure if you’re experiencing them, consult your doctor.
How to Raise Blood Glucose Levels
If you’re experiencing low blood sugar or hypoglycemia, it’s important to take steps to raise your blood sugar levels. Some general steps to take are,
1. Follow the 15-15 Rule:
This rule is commonly recommended for treating low blood sugar. It involves eating 15 grams of carbohydrates, waiting 15 minutes, and then checking your blood sugar again.
Foods that contain 15 grams of carbohydrates include:
- Glucose tablets (follow package instructions)
- 1/2 cup (4 oz) of fruit juice or regular (not diet) soda
- 1 tablespoon of honey or sugar
- Hard candies, jellybeans, or gumdrops (see package for content)
2. Retest Your Blood Sugar:
After waiting about 15 minutes, check your blood sugar level again.
3. Eat a Snack or Meal:
If your next meal is more than an hour or two away, eat a small snack after you’ve raised your blood sugar to a safe level.
This can help stabilize your blood sugar levels until your next meal. The snack should contain protein and carbohydrates.
For example, crackers with cheese or half a sandwich could work.
Remember, if you have diabetes or another health condition that puts you at risk for hypoglycemia, you should always have a source of fast-acting carbohydrates on hand.
Don’t let it go out of hand, as your bystanders have to activate the emergency Response system to call an ambulance, as it is a Medical Emergency!
Blood Sugar Levels: Why They Change With Age
Blood sugar levels can change with age due to several reasons:
1. Decreased Muscle Mass:
As people age, they tend to lose muscle mass and gain fat. Since muscle is an important site for insulin-mediated glucose uptake, this shift can lead to decreased insulin sensitivity and increased blood sugar levels.
2. Increased Abdominal Fat:
Aging is often associated with an increase in abdominal fat, which can lead to insulin resistance, a condition in which your body doesn’t use insulin efficiently. This can result in higher blood sugar levels.
3. Decreased Physical Activity:
Many people become less active as they age, which can lead to weight gain and increased blood sugar levels.
4. Changes in Hormone Levels:
Aging can also lead to changes in hormone levels, which can affect how your body processes glucose.
5. Decreased Beta Cell Function:
Beta cells in the pancreas produce insulin. With age, the function of these cells can decline, leading to less insulin production and higher blood sugar levels.
6. Increased Risk of Illness:
The risk of illnesses, including those that can impact blood sugar levels like hypertension and cardiovascular disease, increases with age.
Age-Specific Factors Impacting Blood Sugar Control
1. Lifestyle and Dietary Choices
2. Physiological Changes and Hormonal Factors
3. Comorbidities and Medication
These factors play a significant role in blood sugar control across different age groups:
1. Lifestyle and Dietary Choices
Children and Adolescents:
Diet and lifestyle habits developed in these stages can significantly impact blood glucose control. It’s important to encourage a balanced diet and regular physical activity. Also, adolescents might face unique challenges like peer pressure towards unhealthy food choices and inconsistent schedules.
Adults:
Workplace stress, sedentary lifestyle, and unhealthy dietary choices may lead to weight gain, which can increase the risk of developing type 2 diabetes. Balancing work, family, and health can be challenging, but it’s important for maintaining good glycemic control.
Older Adults:
Changes in taste, dental health, and income may impact diet quality. Reduced mobility or chronic conditions might limit physical activity, potentially worsening glycemic control. Social isolation can also affect meal patterns and nutritional intake.
2. Physiological Changes and Hormonal Factors
Children and Adolescents:
The growth hormone surge during puberty can lead to increased insulin resistance. This, combined with the above lifestyle factors, can increase the risk of developing type 2 diabetes.
Adults:
As adults age, they may experience a gradual increase in weight and loss of muscle mass, leading to increased insulin resistance.
Women in menopause may experience fluctuations in blood glucose levels due to changing hormone levels.
Older Adults:
Aging is associated with decreased muscle mass and increased abdominal fat, which can lead to increased insulin resistance. Aging also brings decreased beta cell function, impacting insulin production and potentially leading to higher blood sugar levels.
3. Comorbidities and Medication
Children and Adolescents:
While generally less common in this age group, some children and adolescents may have comorbidities or require medications that can impact blood sugar control.
Adults:
The presence of comorbidities such as obesity, hypertension, or dyslipidemia can affect blood sugar control. Additionally, some medications for these conditions may impact blood glucose levels.
Older Adults:
Older adults often have multiple comorbidities that require various medications, which can affect blood glucose control. Conditions like dementia might also affect their ability to manage diabetes.
In each of these stages, personalized care and regular medical check-ups are crucial for managing blood glucose levels effectively.
Blood Sugar in the Elderly: Risks, Recommendations and Diabetes Management
Managing blood sugar levels in the elderly population can be challenging due to age-related physiological changes, comorbidities, and the use of multiple medications. Here are some risks, recommendations, and strategies for diabetes management in older adults:
Risks:
1. Hypoglycemia:
Older adults are at a higher risk of hypoglycemia (low blood sugar) due to factors like decreased renal function, poor nutritional status, and the use of certain medications.
2. Hyperglycemia:
On the other hand, decreased physical activity, increased abdominal fat, and loss of lean muscle mass can lead to insulin resistance and hyperglycemia (high blood sugar).
3. Complications:
Poorly controlled diabetes can lead to complications like heart disease, stroke, kidney disease, vision problems, and nerve damage, which can significantly impact an older adult’s quality of life.
Recommendations and Diabetes Management:
1. Personalized Care: Due to the complex health issues in older adults, diabetes care should be individualized, taking into account the person’s overall health, cognitive function, physical abilities, and personal preferences.
2. Diet and Exercise: A balanced diet and regular physical activity can help control blood sugar levels. For older adults with limited mobility, activities like chair exercises or walking can be beneficial.
3. Medication Management: It’s crucial to manage medications effectively, considering potential side effects and interactions that can affect blood sugar levels. Sometimes, simplifying the medication regimen can help with adherence.
4. Regular Monitoring: Regular monitoring of blood sugar levels is important. Blood glucose targets might be relaxed compared to younger adults, to prevent hypoglycemia.
5. Comorbidity Management: It’s important to manage other coexisting conditions, like hypertension or heart disease, which can impact blood sugar control and increase the risk of diabetes complications.
6. Support and Education: Provide education about diabetes management, and ensure they have support, either from family members or caregivers, especially if they have cognitive impairment or difficulty with self-care.
Regular check-ups with a healthcare provider and routine screening for diabetes complications can help manage blood sugar levels and maintain the best possible quality of life for older adults with diabetes.
Future of Blood Sugar Monitoring: Innovations and Trends
Innovations that can change the way, Blood Glucose is Monitored are,
1. Continuous Glucose Monitors (CGMs):
CGMs have already revolutionized blood glucose monitoring by providing real-time, around-the-clock readings. They offer trend data, hypo and hyperglycemia alerts, and can reduce the need for frequent finger pricks.
Future advancements are likely to make CGMs more accurate, affordable, and user-friendly.
2. Non-Invasive Glucose Monitors:
Researchers are exploring non-invasive methods for monitoring blood glucose levels, such as devices that use light (spectroscopy), electricity (impedance), or even sound waves (ultrasound).
While none of these technologies have been perfected yet, their development is an exciting prospect for pain-free glucose monitoring.
3. Smart Insulin Pens and Pumps:
Future insulin delivery devices will likely have more advanced features, such as the ability to sync with smartphone apps or CGMs, automated insulin delivery based on glucose readings, and more precise dosing options.
4. Artificial Pancreas Systems:
Also known as closed-loop systems, these combine CGMs and insulin pumps to automatically adjust insulin delivery based on current glucose levels.
This can help minimize the burden of managing blood sugar levels and reduce the risk of hypoglycemia and hyperglycemia.
5. Data Analytics and Digital Health:
With the rise of health data and smart devices, there’s a growing focus on how to use this data to improve diabetes care.
This includes personalized treatment plans, predictive analytics (e.g., predicting hypoglycemia before it happens), and integrating glucose data with other health data for a more comprehensive view of the individual’s health.
6. Glucose-Sensing Smart Contact Lenses:
Although still in the research phase, smart contact lenses that can monitor glucose levels in tears could offer another non-invasive option for people with diabetes.
7. Implantable Glucose Sensors:
Future developments may see the rise of implantable glucose sensors that could provide continuous monitoring for a year or more without replacement.
Remember, while these innovations show promise, not all of them might become commercially available, and those that do will need to go through rigorous testing to ensure their accuracy, safety, and effectiveness.
Frequently Asked Questions
What Is The Normal Blood Sugar Level For Diabetic Patients?
The normal blood sugar level for diabetic patients typically is around 70 to 130 mg/dL before meals, and less than 180 mg/dL about 1 to 2 hours after starting a meal.
However, these values may vary based on individual health conditions and treatment goals, so it’s always best to discuss with your Doctor.
What Is The Normal Range For Diabetes According To Age?
The normal range for blood glucose levels tends to stay consistent across all ages. For a non-diabetic person, fasting blood glucose levels are generally between 70 and 100 mg/dL.
For people with diabetes, specific blood glucose targets are individualized based on several factors, including age, but overall health, the presence of other diseases, and risk of hypoglycemia are also considered.
Is 200 Blood Sugar Normal After Eating?
A blood sugar level of 200 mg/dL or higher after eating may indicate hyperglycemia, particularly if these readings are consistent or accompanied by diabetes symptoms. It’s advisable to consult a healthcare provider for an evaluation in this case.
Is 250 Sugar Level Normal?
A blood sugar level of 250 mg/dL is considered high. If it occurs frequently, it could be indicative of poorly controlled diabetes, and you should seek medical advice.
What Is The Highest Sugar Level For Diabetes?
There isn’t a “highest” sugar level for diabetes as such, but a blood sugar level of 200 mg/dL or more typically indicates diabetes. However, extremely high blood sugar levels (for example, over 600 mg/dL) can cause a serious condition called diabetic ketoacidosis in type 1 diabetes or hyperosmolar hyperglycemic state in type 2 diabetes, both of which are medical emergencies.
Is 300 Sugar Levels High?
Yes, a blood sugar level of 300 mg/dL is considered high and can cause serious symptoms. If a person’s blood sugar levels frequently rise to 300 mg/dL, it suggests their diabetes is not well controlled and requires immediate medical attention.
What Age Group Is Most Commonly Affected By Diabetes?
The risk of developing type 2 diabetes increases with age, particularly after the age of 45. However, it’s important to note that type 2 diabetes is increasingly being diagnosed in younger people due to lifestyle factors.
What Is Normal HbA1c By Age?
HbA1c, or glycated hemoglobin, levels are typically below 5.7% for non-diabetic adults. For people with diabetes, a common target is less than 7%, although this can vary based on the individual’s health status and the advice of their healthcare provider.
These targets don’t typically change with age, but older adults might have slightly relaxed targets to prevent hypoglycemia.
Is Blood Sugar Higher With Age?
Blood sugar levels can become harder to control with age due to factors like increased abdominal fat, decreased muscle mass, and other physiological changes associated with aging.
Can Type 2 Diabetes Be Cured?
Type 2 diabetes is generally considered a chronic condition that can be managed but not cured. Lifestyle modifications and medication can effectively manage symptoms and prevent complications, but ongoing treatment is typically necessary.
Some individuals may achieve “remission” where their blood sugar levels remain normal without the need for diabetes medication, but this isn’t the same as a cure, and regular health monitoring is still essential.
Significant Weight Loss has also shown to reverse Diabetes in the early stages, Consult and Discuss it with your Doctor
Is 250 Blood Sugar High After Eating?
Yes, a blood sugar level of 250 mg/dL after eating is considered high. Normal blood sugar levels for people without diabetes are typically less than 140 mg/dL after eating. If you’re consistently experiencing such high readings, it’s important to consult your doctor.
Is 200 Too High For A Diabetic?
A blood sugar level of 200 mg/dL or higher is typically considered high, even for individuals with diabetes. Regular readings at this level suggest that the diabetes may not be well controlled, and you should discuss this with your healthcare provider.
How Can I Reduce My Sugar Level Fast?
Quick ways to lower blood sugar levels include exercise, drinking plenty of water to help remove excess glucose through urine, and modifying your diet to include fewer carbohydrates and more fiber.
If your blood sugar levels are frequently high, however, you should discuss long-term management strategies with your diabetologist.
What Is The Best Treatment Of Diabetes?
The best treatment for diabetes is a combination of a healthy diet, regular physical activity, medication or insulin as prescribed, and regular monitoring of blood sugar levels.
Treatment plans should be individualized based on the person’s overall health, type of diabetes, and lifestyle.
How Can I Control My Sugar Naturally?
Natural ways to control blood sugar include regular exercise, a balanced diet rich in fiber and low in refined carbohydrates, maintaining a healthy weight, getting adequate sleep, and managing stress levels.
What Is A Normal Blood Sugar Level After Fasting For 8 Hours?
A normal fasting blood sugar level for a non-diabetic person is typically between 70 and 100 mg/dL.
What Is Normal Sugar Level By Age?
Blood sugar levels don’t generally vary by age.
For non-diabetic individuals, fasting blood glucose levels are usually between 70 and 100 mg/dL, and post-meal levels are typically less than 140 mg/dL.
Target levels for people with diabetes can vary based on individual health concerns and treatment goals.
What Is Normal Sugar Level Before Food?
For a non-diabetic person, normal blood sugar levels before meals are usually between 70 and 100 mg/dL. For people with diabetes, a common target is between 80 and 130 mg/dL, but this can vary based on individual health conditions and treatment goals.
What Is A Good Blood Sugar Level In The Morning?
A good fasting blood sugar level (morning level, before eating) is typically between 70 and 100 mg/dL for non-diabetic people.
For people with diabetes, a common target is between 80 and 130 mg/dL, but this can vary based on individual health factors.
Is 135 Blood Sugar High In The Morning?
A fasting (morning) blood sugar level of 135 mg/dL is considered high for both diabetic and non-diabetic individuals.
If you consistently have readings at this level in the morning, it’s important to discuss this with your healthcare provider.
Is Fasting Sugar 110 Normal?
A fasting blood sugar level of 110 mg/dL is slightly elevated for a non-diabetic person, as normal fasting blood glucose levels are typically between 70 and 100 mg/dL.
If you frequently have fasting blood sugar readings at this level, it’s advisable to discuss this with a healthcare provider.
What Is The Best Time To Check Your Blood Sugar Level?
The best time to check blood sugar depends on your goals for testing.
Common times include before meals (to help decide how much insulin to take, if you take insulin), about 2 hours after meals (to see how your body handles the food), and before bedtime.
Some people also need to test in the middle of the night. Your healthcare provider can help you decide when to test.
What Is The Normal Sugar Level For Non-Diabetic?
For non-diabetic individuals, fasting blood glucose levels are typically between 70 and 100 mg/dL. About 2 hours after starting a meal, blood sugar levels are typically less than 140 mg/dL.
What Blood Sugar Should You Go To The Hospital For?
A blood sugar level above 300 mg/dL could be dangerous and warrant a trip to the hospital, especially if it’s accompanied by symptoms of hyperglycemia like excessive thirst, frequent urination, confusion, or fruity-smelling breath.
Additionally, any level above 240 mg/dL along with the presence of ketones in urine is a sign of ketoacidosis, a potentially life-threatening condition that requires immediate medical attention.
Is 200 Blood Sugar Normal After Eating?
A blood sugar level of 200 mg/dL or higher after eating is considered high for both individuals with and without diabetes. Regular readings at this level suggest that your body isn’t effectively managing blood glucose and you should consult your healthcare provider.
How Soon After Waking Up Should I Test My Blood Sugar?
Testing your blood sugar as soon as you wake up gives you a measurement of your fasting blood sugar level, which can be a useful piece of information for managing your diabetes. This should be done before you eat, drink, or exercise in the morning.
What Is The Normal Blood Sugar Level For A 5 Year Old Child?
For children without diabetes, normal blood sugar levels are typically between 70 and 150 mg/dL, regardless of when they last ate.
For children with diabetes, blood sugar targets are individualized based on the child’s age, duration of diabetes, ability to recognize hypoglycemia symptoms, and other factors.
Is 150 A High Blood Sugar Level?
A blood sugar level of 150 mg/dL is considered high for a fasting reading. However, this level might be seen as normal or near-normal for a reading taken after a meal.
What Is The Highest Blood Sugar Level That Is Safe?
There’s no universally “safe” upper limit for blood sugar. For non-diabetic individuals, blood sugar levels typically remain below 140 mg/dL even after eating.
For those with diabetes, a common post-meal target is less than 180 mg/dL. Consistently higher readings suggest that the diabetes isn’t well controlled.
What Should Blood Sugar Be At Bedtime?
For non-diabetic individuals, bedtime blood sugar levels are typically between 70 and 100 mg/dL. For those with diabetes, a common target is between 100 and 140 mg/dL, but this can vary based on individual health conditions and treatment goals.
What Is A Normal Sugar Level For A Man?
Blood sugar levels do not significantly differ between genders. For non-diabetic men, fasting blood glucose levels are typically between 70 and 100 mg/dL, and post-meal levels are typically less than 140 mg/dL.
Is 139 High For Blood Sugar?
A blood sugar reading of 139 mg/dL is slightly high if it’s a fasting reading. However, this level would be within the normal range for a reading taken after a meal.
What Level Of Blood Sugar Is Dangerous?
Blood sugar levels above 180 mg/dL are generally considered high, while readings above 240 mg/dL can be dangerous, particularly if they are accompanied by symptoms of hyperglycemia.
Levels above 300 mg/dL or any level above 240 mg/dL with the presence of ketones in the urine could be life-threatening and require immediate medical attention.
When Is Blood Sugar Level High?
For non-diabetic individuals, a blood sugar level is considered high if it’s over 100 mg/dL after an overnight fast or over 140 mg/dL two hours after eating.
For those with diabetes, the thresholds are typically higher. Fasting blood sugar above 130 mg/dL or a reading over 180 mg/dL after a meal might be considered high.
For A Diabetic Patient, What Are The Three Medical Emergencies?
The three primary medical emergencies for a person with diabetes are severe hypoglycemia (blood sugar too low), diabetic ketoacidosis (DKA), and hyperosmolar hyperglycemic state (HHS).
Each of these conditions is serious and requires immediate medical attention.
What Is The Random Blood Sugar Level?
A random blood sugar level is a blood glucose test taken at any time, regardless of when you last ate. The normal range for a random blood glucose test for a non-diabetic individual is typically less than 140 mg/dL.
What Blood Sugar Level Requires Insulin?
Not all people with high blood sugar need insulin. However, if a person with type 1 diabetes has a blood sugar level above their target range, they’ll likely need insulin.
People with type 2 diabetes might need insulin if their blood sugar isn’t controlled with diet, exercise, and oral medications.
The specific blood sugar level that requires insulin can vary significantly between individuals and should be determined in consultation with a Diabetologist.
Can Covid Increase Blood Sugar Levels?
Yes, any infection, including COVID-19, can increase blood sugar levels. The body’s response to illness or stress often involves releasing hormones that promote glucose production and limit insulin effectiveness.
What Is Considered A Dangerously Low Blood Sugar Level?
A blood sugar level below 70 mg/dL is considered low (hypoglycemia) and could potentially be dangerous. Immediate treatment is typically required to prevent symptoms from worsening.
Do Tomatoes Raise Blood Sugar Levels?
Tomatoes are a low-glycemic food, which means they have a minimal impact on blood sugar levels. Most people can include tomatoes in their diet without worrying about significant blood sugar spikes.
Does Walking Reduce Blood Sugar Levels?
Yes, physical activity like walking can help lower blood sugar levels by encouraging your muscles to use glucose for energy. Regular exercise is an important part of managing blood glucose levels and overall health for those with and without diabetes.
How To Lower Blood Sugar Levels For Type 2 Diabetes?
Lowering blood sugar levels in type 2 diabetes involves a combination of lifestyle changes and medication.
Lifestyle changes include adopting a healthy diet that is low in simple sugars and high in fiber, regular physical activity, maintaining a healthy weight, and monitoring blood sugar levels.
Medication may include oral drugs like metformin or insulin injections. It’s also important to manage stress levels and get adequate sleep.
What Hormone Controls Blood Sugar Levels?
Insulin is the primary hormone that controls blood sugar levels. Produced by the pancreas, insulin allows cells to take in glucose from the bloodstream for energy.
Another hormone, glucagon, works in opposition to insulin, raising blood sugar levels by encouraging the liver to convert stored glycogen into glucose.
What Is The Ideal Blood Sugar Level For My Age?
Blood sugar levels typically don’t vary with age. For non-diabetic individuals, fasting blood glucose levels are usually between 70 and 100 mg/dL, and post-meal levels are typically less than 140 mg/dL.
However, for people with diabetes, the target blood sugar levels can vary based on individual health conditions, complications risk, and treatment goals.
How Does Aging Affect Blood Sugar Control?
Aging can affect blood sugar control in several ways. Muscle mass decreases with age, which can reduce the amount of glucose that’s removed from the bloodstream.
The body’s cells may also become less sensitive to insulin, a condition known as insulin resistance. Additionally, the pancreas may produce less insulin as you age.
What Are The Best Strategies To Manage Blood Sugar Levels As I Age?
Good strategies include regular physical activity, maintaining a healthy weight, eating a balanced diet, and monitoring blood sugar levels regularly.
It’s also important to manage other health conditions that could affect blood sugar control, such as high blood pressure and high cholesterol, and to work closely with your healthcare provider to adjust your treatment plan as needed.
What Role Does Technology Play In Monitoring Blood Sugar Levels?
Technology plays a significant role in monitoring blood sugar levels. Glucose meters allow for regular at-home testing, while continuous glucose monitors (CGMs) can provide nearly real-time tracking of glucose levels.
Insulin pumps can deliver insulin more precisely, and some can even respond to changes in blood sugar levels automatically.
How Do I Set Individualized Glycemic Goals?
Individualized glycemic goals should be set in consultation with your healthcare provider.
They will consider factors such as your age, how long you’ve had diabetes, your overall health, the presence of any diabetes complications, and your personal lifestyle when setting these goals.
They will also consider your ability to safely achieve these goals.